Introduction to Different Types of Dentures
Modern dentures are more comfortable, convenient, and realistic than ever before. If you believe dentures might be a right fit for you, contact Grandview Dental Care.

Modern dentures are more comfortable, convenient, and realistic than ever before. If you believe dentures might be a right fit for you, contact Grandview Dental Care.

Invisalign® revolutionized the way people look at orthodontic treatment. Learn how the clear aligner system from Invisalign® made it possible for people to discreetly improve their smiles.
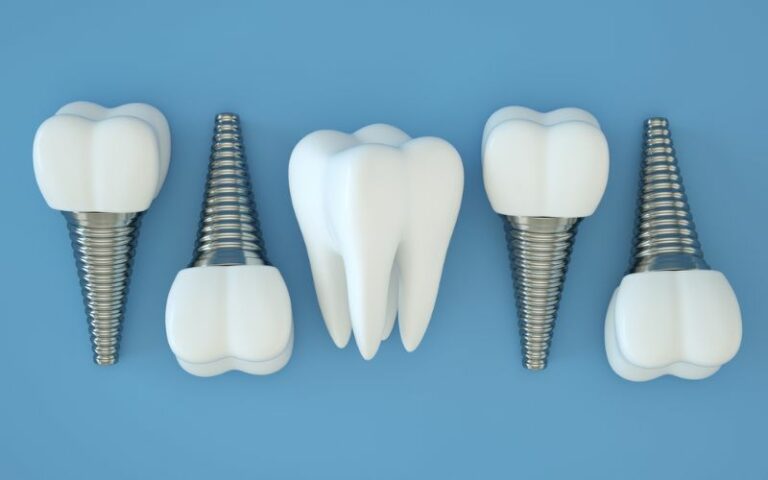
Dental implants are used to support the replacement of a single tooth or multiple teeth depending on the individual’s requirements and condition. Reading about the pros and cons of the process may help you decide if dental implants are right for you.
1220 Grandview Ave
Columbus, OH, 43212
View Map
Monday: 9am - 5pm
Tuesday: 8am - 6pm
Wednesday: 8am - 6pm
Thursday: 8am - 4pm
Friday: 8am - 2pm